How Accurate Are CGMs? New Study and Key Takeaways

Are CGMs accurate?
CGM data is at least slightly delayed because these devices gather data from the interstitial fluid rather than the blood itself (more on that later).
Additionally, a 2025 study published in The American Journal of Clinical Nutrition provides new insights suggesting that CGM readings can sometimes overestimate glucose levels, particularly after meals.
In this article, we’ll break down the science behind CGM accuracy, explain why readings can vary from person to person, and provide practical tips for interpreting your results correctly.
How a CGM Works and Why Accuracy Varies
When you look at a CGM reading, you’re not seeing the raw chemical signal from the sensor.
Instead, you’re seeing the device’s best estimate of your glucose at that moment.
The reason you don’t see the raw, unprocessed signal is that it’s extremely sensitive to a lot of non-glucose factors, like:
- Temperature
- Pressure on the sensor
- Slight shifts in sensor chemistry over time
- Minor motion artifacts
If you just saw the raw signal, the numbers would jump around constantly and would be more misleading than helpful.
Additionally, the sensor measures the glucose in the interstitial fluid rather than the blood.
This is important because there’s a natural lag from the time the glucose diffuses from the blood to the interstitial fluid.
This delay usually ranges from 5 to 25 minutes.
Unfortunately, the time delay varies depending on many factors, like:
- Hydration
- The speed at which your body digests food
- The type of food consumed (carbs, fiber, fat content)
The algorithms in modern CGMs are designed to account for these nuances and provide near real-time estimates, even when glucose is rising or falling quickly.
However, there’s certainly room for error, and readings can vary between people and across different meals.
Factors like hydration, skin thickness, and the speed at which glucose enters the bloodstream can influence how closely the CGM reflects your true blood glucose.
Some glucose monitors allow you to calibrate them with a finger prick to improve accuracy (as studies show the finger prick is fairly accurate), though this isn’t always available.
What is MARD?
MARD (Mean Absolute Relative Difference) is the standard metric used to evaluate a CGM’s accuracy.
This metric indicates how closely a CGM’s readings match a lab reference value, expressed as a percentage. For example, a MARD of 10% means the CGM is, on average, within 10% of the reference value.
The lower the MARD, the more accurate the CGM is.
According to a recent paper in Diabetes Technology & Therapeutics, a MARD of less than 10% is considered good.
It sounds straightforward, but the source also argues that MARD is often misunderstood and even misleading.
Accuracy isn’t a single fixed number. As alluded to earlier, MARD can vary depending on:
- Who’s wearing the sensor: People with type 1 versus type 2 diabetes, or non-diabetics.
- Where the sensor is placed: Arm versus the abdomen.
- The glucose range measured: Accuracy tends to be different at very low versus very high glucose levels.
- The time since insertion: Accuracy can shift during the first 12-24 hours of wear.
In other words, MARD gives a rough ballpark, but it doesn’t capture the whole story of how a CGM will behave in everyday life.
To make this more concrete, a 2024 study in the Journal of Diabetes Science and Technology compared two of the newest sensors: the Dexcom G7 and the Abbott FreeStyle Libre 3.
Both were tested in adults with diabetes, and here’s what they found:
- Overall accuracy: Libre 3 showed a lower MARD (≈10%) compared to Dexcom G7 (≈15%) over the course of the study.
- Early wear: In the first 12 hours, the two devices performed similarly. After that, Libre 3 was consistently more accurate.
- Within-range readings: 91.4% of Libre 3 readings fell within ±20 mg/dL of the reference, compared to 78.6% for Dexcom G7.
This highlights two important points.
First, different devices vary in accuracy, even among the most advanced models.
Secondly, MARD isn’t the whole picture because even if a device looks “accurate on average,” it could still struggle in critical situations like during rapid glucose spikes, overnight lows, or the first day after insertion, which are often the moments people care about most.
Nevertheless, MARD is still the common metric used to gauge CGM accuracy, and here’s a table that shows an overview of the MARD scores for various popular CGMs:
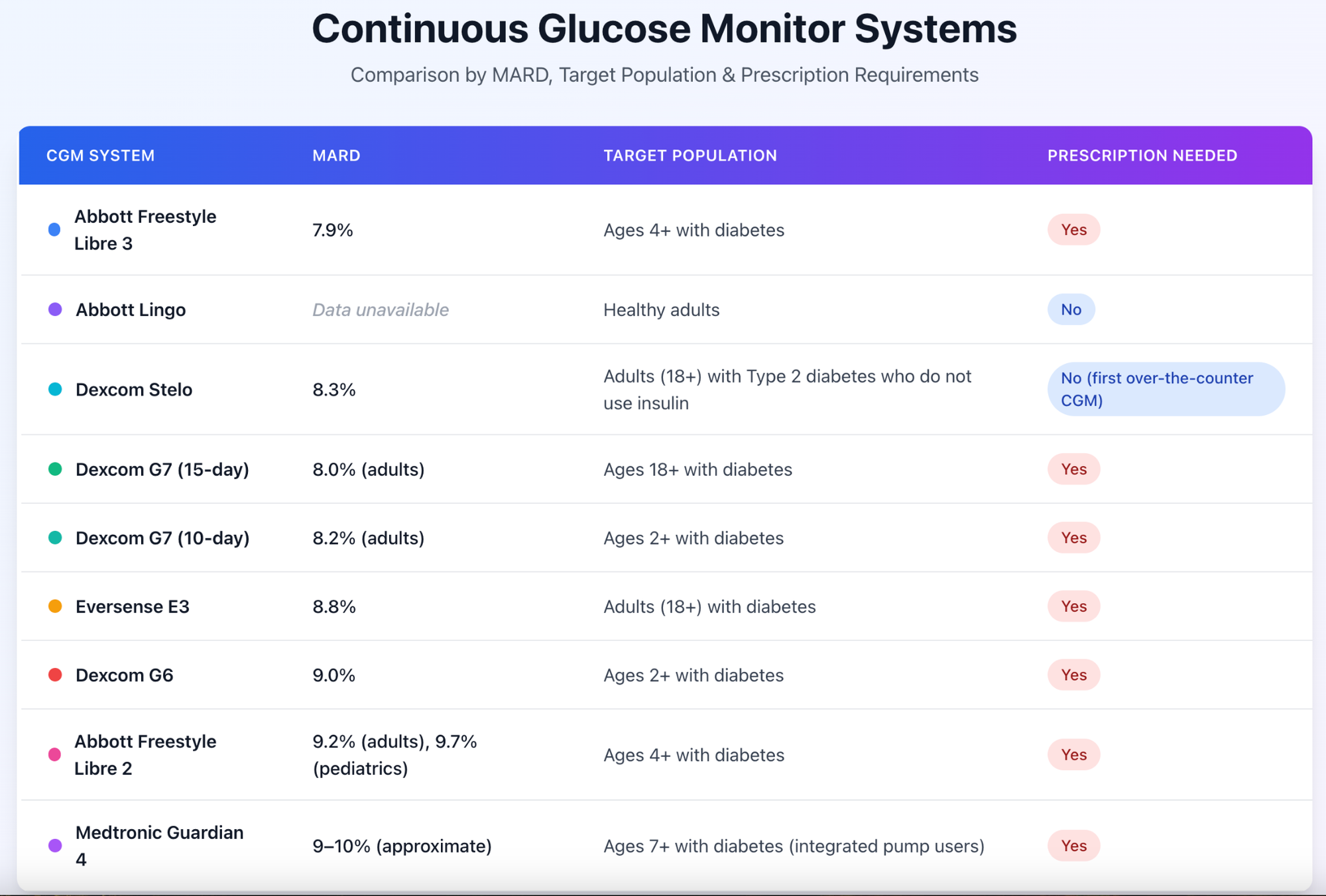
Here’s another visualization of the different MARD scores for these common CGMs:
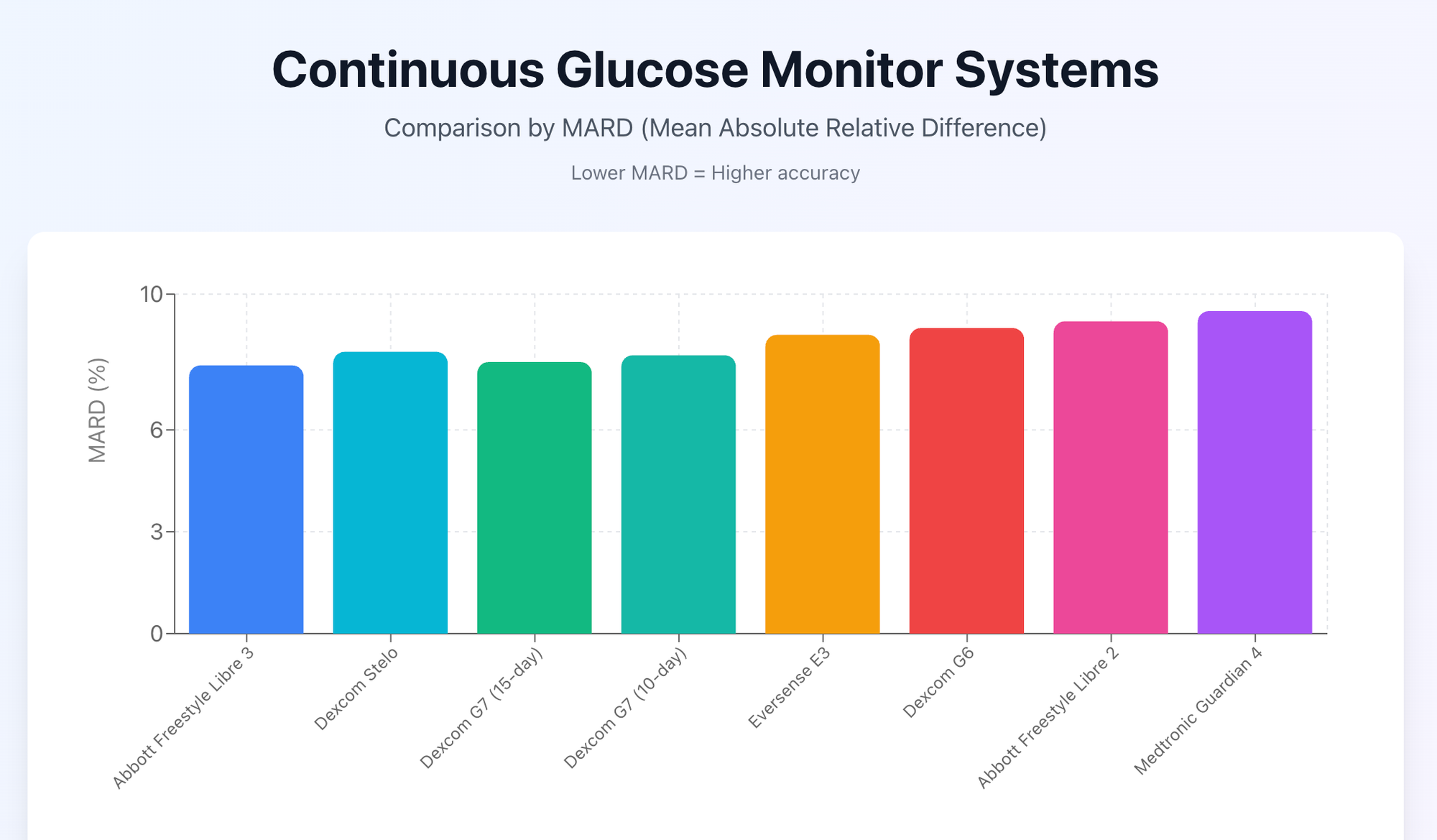
An Overview of Key Factors That Impact CGM Accuracy
To summarize the factors we’ve discussed thus far, here’s an overview of key variables that impact CGM accuracy:

Practical Takeaways for Non-Diabetics
Even if CGMs aren’t 100% accurate, they’re still very useful tools to improve your general health and fitness.
Now that we know CGMs can slightly overestimate glucose, especially after meals, here are some actionable takeaways for non-diabetics to effectively use this data.
Track Patterns Related to Exercise and Food
Instead of stressing over whether your CGM reads 120 mg/dL or 104 mg/dL, look at how your glucose rises and falls throughout the day.
Do you notice certain foods consistently causing bigger spikes than others?
How do you notice that specific workouts consistently lower your glucose more than others?
These trends can give you plenty of useful information to improve your health and fitness.
Consider the Timing of Readings
As CGMs measure glucose in the interstitial fluid, there’s a natural lag of roughly 5-25 minutes compared to blood glucose.
Unfortunately, the CGM algorithm can’t predict this spike, so your CGM is likely reflecting blood sugar levels from a few minutes earlier. Keep this lag in mind when making real-time decisions, like whether to eat a snack or adjust your workout intensity.
Consider Context Beyond Food and Exercise
If you just finished a workout and your CGM shows a higher-than-expected reading, it might be partly due to temporary changes in blood flow or sweat affecting the sensor.
Or if you’re dehydrated, glucose in your interstitial fluid can appear slightly elevated compared to your actual blood glucose.
Even stress or lack of sleep can cause cortisol-driven glucose spikes that aren’t tied to food. So, before making a judgment like cutting out a meal, consider other factors.
Here’s a quick cheat sheet:
- Sleep
- Hydration
- Stress
- Temperature
Calibration Helps
If your device allows for finger-prick calibration, using it occasionally can improve accuracy. Yet even without calibration, CGMs still provide incredibly useful trend information that can help you make smarter choices over time.
Even if your CGM doesn’t allow you to calibrate it, you can use a finger prick to occasionally compare the data and better estimate your real glucose levels.
How to Make The Most of Your CGM
CGMs are highly useful for tracking trends, identifying foods that spike blood sugar, and monitoring your workouts and recovery.
However, you still might need someone to hold you accountable to the data.
That’s where a program like Wearable Challenge can help.
You stake $20/day to stay under a healthy glucose threshold and therefore avoid major spikes and crashes.
This creates meaningful accountability while also learning about how your body responds to certain foods. Join Wearable Challenge today to transform your CGM data into action.